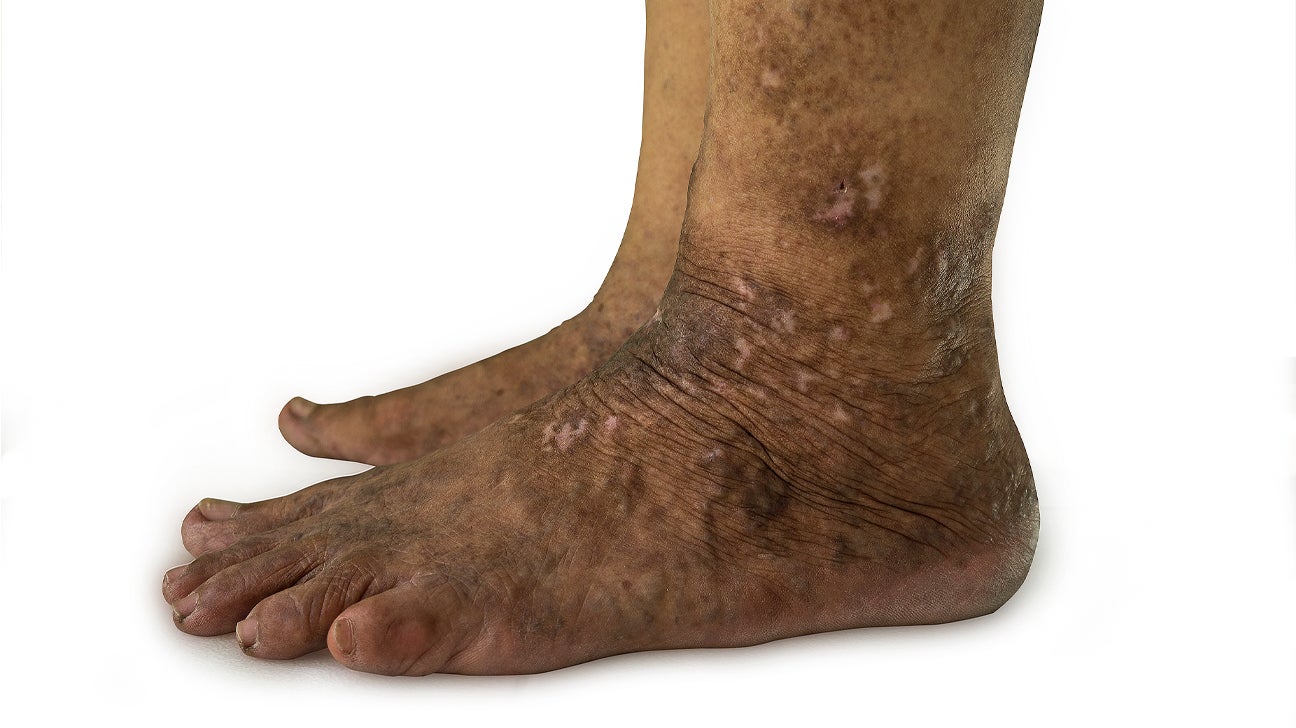
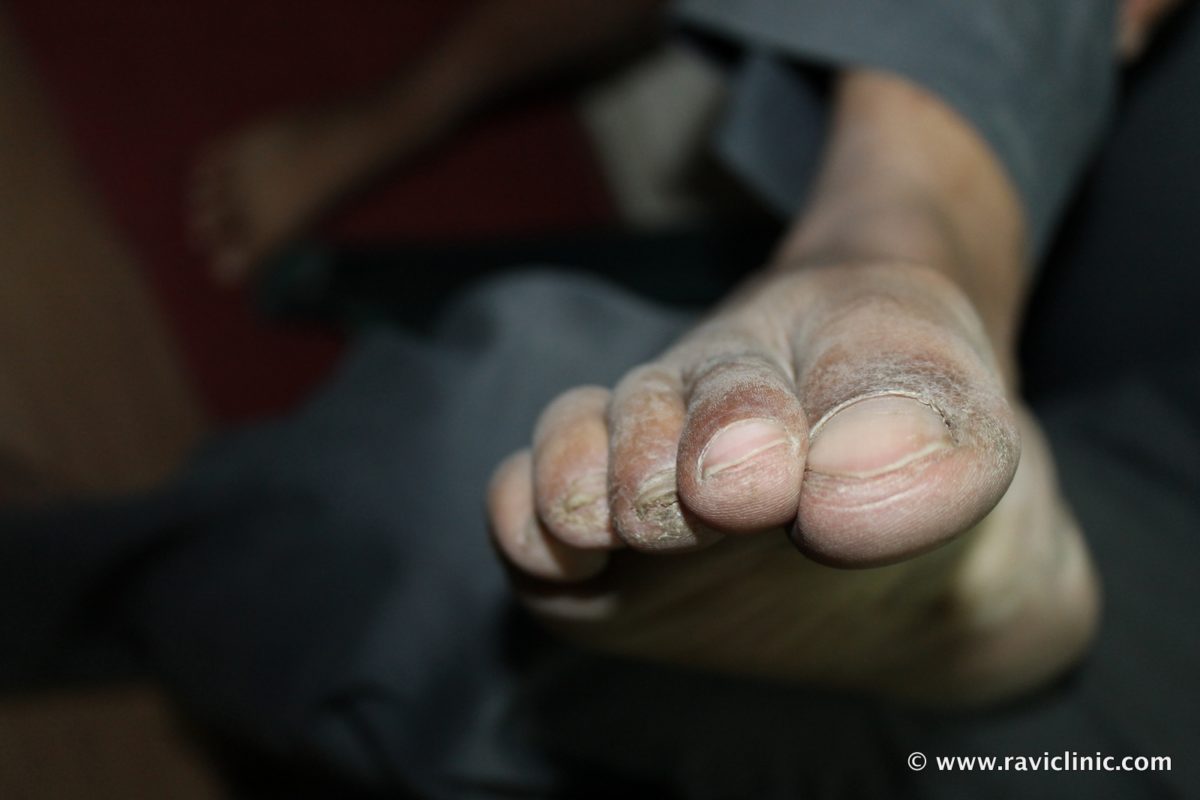
Psoriasis on feet is a common and often misunderstood skin condition that affects millions of people worldwide. This chronic autoimmune disorder can significantly impact an individual's quality of life, making it crucial to understand its causes, symptoms, and treatment options. In this article, we will delve into the complexities of psoriasis on feet, providing comprehensive insights and actionable advice for those seeking relief.
Psoriasis is more than just a skin condition; it is a lifelong battle that requires a deep understanding of its underlying causes and triggers. Whether you're newly diagnosed or have been living with psoriasis for years, gaining knowledge about its effects on the feet can empower you to take control of your health.
This article will explore everything you need to know about psoriasis on feet, from its symptoms and treatment options to lifestyle changes that can help manage the condition effectively. By the end of this guide, you'll have a clearer understanding of how to navigate this challenging skin disorder.
Read also:Liberty Vs Mercury A Comprehensive Comparison Of Two Iconic Symbols
Table of Contents
- What is Psoriasis on Feet?
- Common Symptoms of Psoriasis on Feet
- Causes and Triggers of Psoriasis on Feet
- The Diagnosis Process
- Treatment Options for Psoriasis on Feet
- Lifestyle Management and Prevention
- Natural Remedies for Psoriasis on Feet
- Psychological Impact of Psoriasis
- Expert Advice for Managing Psoriasis
- Conclusion: Taking Control of Your Health
What is Psoriasis on Feet?
Psoriasis on feet refers to the appearance of thick, scaly patches on the skin of the feet due to an abnormal immune response. This condition is characterized by rapid skin cell growth, leading to the buildup of dead skin cells on the surface. Unlike other forms of psoriasis, psoriasis on feet can be particularly uncomfortable, affecting mobility and causing significant discomfort.
Types of Psoriasis That Affect Feet
- Plaque Psoriasis: The most common type, characterized by red, raised patches covered with silvery scales.
- Guttate Psoriasis: Smaller, drop-like lesions that may appear after an infection.
- Pustular Psoriasis: Rare but severe, marked by pus-filled blisters.
Understanding the specific type of psoriasis affecting your feet is essential for effective treatment and management.
Common Symptoms of Psoriasis on Feet
The symptoms of psoriasis on feet can vary from person to person, but common signs include:
- Red, inflamed patches on the soles or sides of the feet.
- Thick, silvery scales covering the affected areas.
- Cracked or dry skin that may bleed.
- Itching, burning, or soreness in the affected areas.
- Swollen or stiff joints, which may indicate psoriatic arthritis.
Recognizing these symptoms early can help you seek appropriate treatment and prevent complications.
Causes and Triggers of Psoriasis on Feet
While the exact cause of psoriasis remains unknown, research suggests that it is linked to an overactive immune system. In psoriasis, the immune system mistakenly attacks healthy skin cells, accelerating their growth cycle. This leads to the buildup of dead skin cells on the surface, forming the characteristic plaques.
Read also:What Temperature For Rare Steak The Ultimate Guide To Perfectly Cooked Steak
Common Triggers for Psoriasis on Feet
- Infections, such as strep throat or skin injuries.
- Stress, which can exacerbate symptoms.
- Certain medications, including beta-blockers and lithium.
- Smoking and excessive alcohol consumption.
- Weather changes, particularly cold and dry conditions.
Identifying your personal triggers can help you manage flare-ups more effectively.
The Diagnosis Process
Diagnosing psoriasis on feet typically involves a thorough examination by a healthcare professional. A dermatologist may assess the appearance of the affected skin and ask about your medical history. In some cases, a skin biopsy may be performed to confirm the diagnosis.
Importance of Early Diagnosis
Early diagnosis is crucial for managing psoriasis effectively. It allows for timely intervention and the implementation of a tailored treatment plan. If you suspect you have psoriasis on your feet, consult a healthcare professional as soon as possible.
Treatment Options for Psoriasis on Feet
Treatment for psoriasis on feet depends on the severity of the condition and the individual's response to therapy. Common treatment options include:
- Topical Treatments: Creams and ointments containing corticosteroids, vitamin D analogs, or retinoids.
- Phototherapy: Exposure to controlled doses of UV light to reduce inflammation.
- Oral or Injectable Medications: Systemic drugs such as methotrexate or biologics for severe cases.
Emerging Treatments
Recent advancements in psoriasis treatment have introduced biologic therapies targeting specific immune system pathways. These treatments have shown promising results in managing severe psoriasis on feet.
Lifestyle Management and Prevention
Managing psoriasis on feet involves more than just medical treatment. Lifestyle changes can play a significant role in reducing symptoms and preventing flare-ups.
Tips for Managing Psoriasis on Feet
- Maintain good foot hygiene by washing and moisturizing regularly.
- Wear comfortable, breathable footwear to minimize irritation.
- Engage in stress-reducing activities such as yoga or meditation.
- Follow a balanced diet rich in anti-inflammatory foods like fruits, vegetables, and omega-3 fatty acids.
By adopting these practices, you can improve your overall well-being and better manage your psoriasis.
Natural Remedies for Psoriasis on Feet
In addition to conventional treatments, some individuals find relief through natural remedies. While these methods should not replace medical advice, they can complement your treatment plan.
- Aloe Vera: Known for its soothing properties, aloe vera gel can help reduce inflammation and itching.
- Oatmeal Baths: Soaking in colloidal oatmeal can relieve dryness and irritation.
- Apple Cider Vinegar: Applied topically, it may help alleviate mild psoriasis symptoms.
Always consult your healthcare provider before trying new remedies, especially if you have sensitive skin.
Psychological Impact of Psoriasis
Living with psoriasis on feet can take a toll on mental health. The visible nature of the condition can lead to feelings of self-consciousness, anxiety, or depression. It is essential to address these emotional challenges alongside physical symptoms.
Seeking Support
Joining a support group or speaking with a therapist can provide valuable emotional support. Connecting with others who understand your experiences can be incredibly empowering.
Expert Advice for Managing Psoriasis
According to the National Psoriasis Foundation, staying informed and proactive is key to managing psoriasis effectively. Regular follow-ups with your healthcare provider, adherence to treatment plans, and open communication about your symptoms can lead to better outcomes.
Key Takeaways
- Stay consistent with your treatment regimen.
- Monitor your triggers and adjust your lifestyle accordingly.
- Seek professional help if your symptoms worsen or affect your mental health.
Conclusion: Taking Control of Your Health
Psoriasis on feet may present challenges, but with the right knowledge and resources, you can manage the condition effectively. By understanding its causes, recognizing symptoms early, and following a comprehensive treatment plan, you can improve your quality of life and regain control over your health.
We encourage you to share your experiences and insights in the comments below. Your feedback can help others who are navigating similar challenges. Additionally, explore our other articles for more information on skin health and wellness. Together, let's create a supportive community for those living with psoriasis.
Remember, you are not alone in this journey. With the right support and resources, you can thrive despite psoriasis on feet.